The Enormous Reach of the Stanford Medicine 25
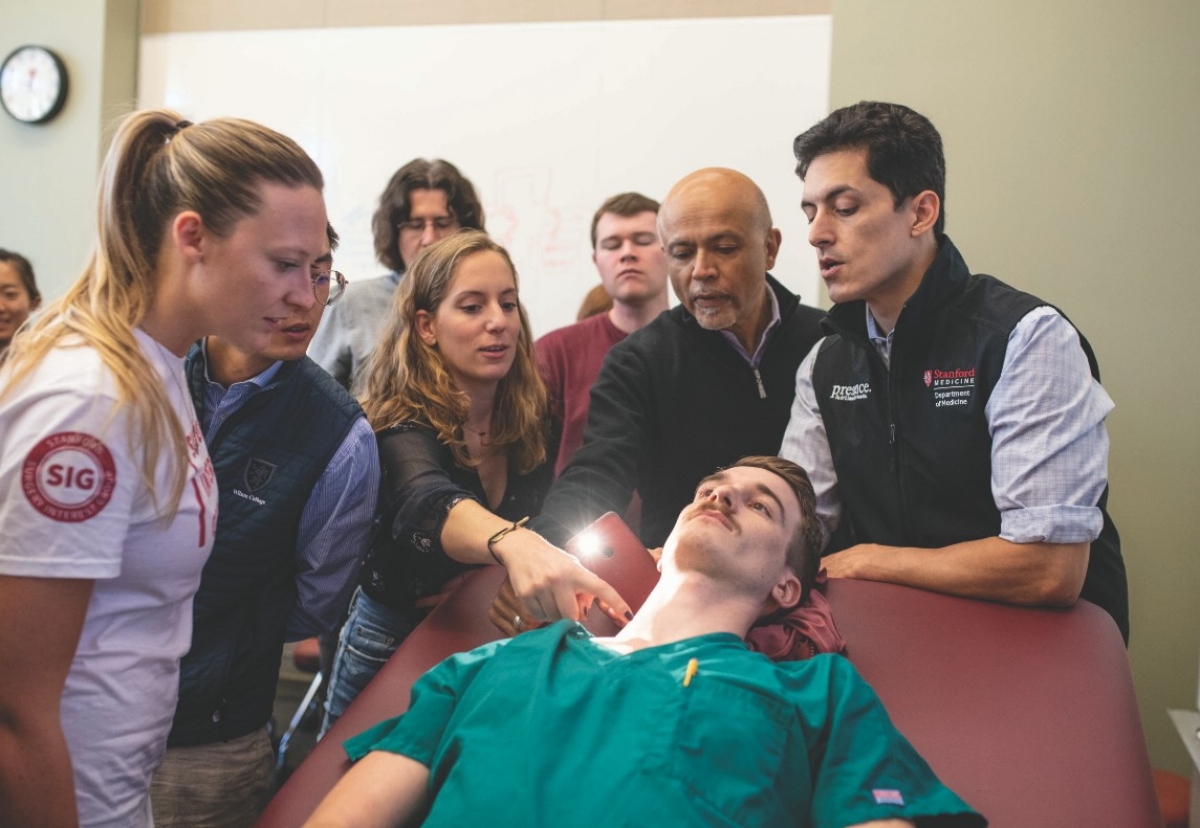
Errol Ozdalga, MD (far right), and Abraham Verghese, MD (holding iPhone), demonstrate one of the Stanford 25 physical diagnosis skills to a group of attentive residents.
The Enormous Reach of the Stanford Medicine 25

Errol Ozdalga, MD (far right), and Abraham Verghese, MD (holding iPhone), demonstrate one of the Stanford 25 physical diagnosis skills to a group of attentive residents.
The Enormous Reach of the Stanford Medicine 25
ONE THING THAT RONALD WITTELES, MD, ASSOCIATE PROFESSOR OF CARDIOVASCULAR MEDICINE, ENJOYS DOING WHEN HE PARTICIPATES IN AN EXCHANGE WITH ANOTHER RESIDENCY PROGRAM IS JOINING MORNING ROUNDS ON THE CARDIAC CARE UNIT (CCU).
As the residency director for the Department of Medicine, he is interested in noting differences between what Stanford residents do on rounds and what residents at other institutions do. As he is a cardiologist, a CCU is familiar territory.
Visiting Yale not long ago, he showed up at the CCU early one morning, unannounced, and walked down a hall to join a group of residents huddled around a computer. To his surprise—and that of the residents once they turned around and noticed him—he saw himself on the screen. The Yale resident group was using the Stanford Medicine 25 website to review proper procedure for measuring a pulsus paradoxus, a rapid fall in blood pressure during inspiration. Witteles had authored the section of the website and been videotaped demonstrating the correct technique.
How the Stanford Medicine 25 Came About
Such an event was never in the mind of Abraham Verghese, MD, vice chair of medicine; John Kugler, MD, clinical associate professor of hospital medicine; and Brooke Cotter, MD, adjunct clinical assistant professor of primary care and population health. Back in 2008 the three shared their concern that bedside physical diagnosis skills taught in the first and second year of medical school are never revisited much after that, not even in the students’ clinical years. As a result, the new interns at Stanford had varied and generally weak bedside exam skills.
“The body is a text and has a story to tell you,” says Verghese, “but you need to be literate, to be able to read the clues. The physical diagnosis maneuvers described in the textbook can appear straightforward on the page, but at the bedside the theoretical knowledge doesn’t help when the technique is poor. Talking about this with John, we had no appetite to teach the whole physical exam course again to interns, and they had no time. But we both wondered, ‘What if we taught them just a few things that were very technique dependent?
Would it not elevate their technique in general?’ It would be like teaching novice cooks 25 involved dishes—they would no doubt also become more comfortable in the kitchen and better appreciate a culinary expert’s skill.”
They settled on what has become the Stanford 25, a set of physical diagnosis skills best taught one on one at the bedside. In the beginning, they taught one such skill in a special session during morning report, then another during another session two weeks later, and so on. It became quite popular, but its principals felt it needed something more.
Moving to the Ether, Reluctantly
They invited some residents to a focus group dinner in Verghese’s apartment and, he says, “I asked them to free associate about the Stanford 25 and tell us what additional things they wanted. The first thing they said they wanted was a website. That was the last thing I wanted; this is all about hands on! But they convinced us that they needed an online correlation to what they were doing with their hands.”
ONE THING THAT RONALD WITTELES, MD, ASSOCIATE PROFESSOR OF CARDIOVASCULAR MEDICINE, ENJOYS DOING WHEN HE PARTICIPATES IN AN EXCHANGE WITH ANOTHER RESIDENCY PROGRAM IS JOINING MORNING ROUNDS ON THE CARDIAC CARE UNIT (CCU).
As the residency director for the Department of Medicine, he is interested in noting differences between what Stanford residents do on rounds and what residents at other institutions do. As he is a cardiologist, a CCU is familiar territory.
Visiting Yale not long ago, he showed up at the CCU early one morning, unannounced, and walked down a hall to join a group of residents huddled around a computer. To his surprise—and that of the residents once they turned around and noticed him—he saw himself on the screen. The Yale resident group was using the Stanford Medicine 25 website to review proper procedure for measuring a pulsus paradoxus, a rapid fall in blood pressure during inspiration. Witteles had authored the section of the website and been videotaped demonstrating the correct technique.
How the Stanford Medicine 25 Came About
Such an event was never in the mind of Abraham Verghese, MD, vice chair of medicine; John Kugler, MD, clinical associate professor of hospital medicine; and Brooke Cotter, MD, adjunct clinical assistant professor of primary care and population health. Back in 2008 the three shared their concern that bedside physical diagnosis skills taught in the first and second year of medical school are never revisited much after that, not even in the students’ clinical years. As a result, the new interns at Stanford had varied and generally weak bedside exam skills.
“The body is a text and has a story to tell you,” says Verghese, “but you need to be literate, to be able to read the clues. The physical diagnosis maneuvers described in the textbook can appear straightforward on the page, but at the bedside the theoretical knowledge doesn’t help when the technique is poor. Talking about this with John, we had no appetite to teach the whole physical exam course again to interns, and they had no time. But we both wondered, ‘What if we taught them just a few things that were very technique dependent? Would it not elevate their technique in general?’ It would be like teaching novice cooks 25 involved dishes—they would no doubt also become more comfortable in the kitchen and better appreciate a culinary expert’s skill.”
They settled on what has become the Stanford 25, a set of physical diagnosis skills best taught one on one at the bedside. In the beginning, they taught one such skill in a special session during morning report, then another during another session two weeks later, and so on. It became quite popular, but its principals felt it needed something more.
Moving to the Ether, Reluctantly
They invited some residents to a focus group dinner in Verghese’s apartment and, he says, “I asked them to free associate about the Stanford 25 and tell us what additional things they wanted. The first thing they said they wanted was a website. That was the last thing I wanted; this is all about hands on! But they convinced us that they needed an online correlation to what they were doing with their hands.”
Blake Charlton, MD, then a medical student and now an interventional cardiology fellow at UC-San Francisco, put together a website during an elective project based on input from Verghese and research on the specific skills. They made basic videos of themselves performing the 25, which were posted on the site.

What Errol has done is truly miraculous, wedding his love of teaching at the bedside with his love of technology
A Further In-Person Enhancement
As the popularity of the Stanford 25 increased, both inside and outside of Stanford, the “bed-med” team sensed a hunger for this applied skill and decided to put on an annual symposium promoting the culture of bedside medicine, with John Kugler taking the lead. The course, now in its fifth year, promised attendees that they would learn to perform and interpret a competent physical exam and, most importantly, to teach advanced physical exam skills at a patient’s bedside.
The popular symposium aims to train clinician-educators who train others at their institutions. “The bedside is where the patients are,” says Verghese, “and we want to show people the joy and renewal that comes from teaching at the bedside and watching students’ eyes open in wonder when we show them how to read the body.”
Focusing on the Website
In 2011, then-third-year resident Errol Ozdalga, MD, offered to take over the website, correcting some errors, revamping the website, and expanding the topics and content. He also created a blog and used social media and other venues to promote the content online to drive more traffic to the site. “I thought if it looked good and made sense,” he says, “people would learn from it.”
He made sure it was widely accessible, and he created many new videos, first working with professional videographers and later doing it himself, from storyboarding to filming and editing, often with other faculty. He then migrated the videos to a YouTube channel. He also committed to having a Stanford 25 session during morning report every other week—without fail—which, says Verghese, “is a major undertaking by itself. And he hasn’t deviated.”
Ozdalga, currently clinical associate professor of hospital medicine and director of the Stanford Medicine 25, discusses another aspect of the Stanford 25: “We involve other faculty from neurology, dermatology, ob/gyn, and many faculty from our medicine department. We also have faculty from outside Stanford, including outside the U.S., whom I have filmed to capture how they teach specific exams. I’m in debt to them all for volunteering time to help grow the content on the website and YouTube channel.”
During a Stanford 25 session, a real patient—as opposed to an actor playing the role of a patient—is often brought in, and the instructors focus on a single element of the physical exam to teach the residents. Ozdalga recalls being “super nervous about teaching my fellow residents a particular skill during a Stanford 25 session. Of course, that’s how you learn: You get thrown in the deep water.”
Today the Stanford 25 website has 5,000 visitors daily and is second only to Stanford’s news office in hits for a Stanford website. In the first six months of 2019, the Stanford 25 website had over 1 million page views: 1.068 million to be precise.
Verghese says, “What Errol has done is truly miraculous, wedding his love of teaching at the bedside with his love of technology. The Stanford 25 is already a well-known go-to resource the world over, but with more resources and personnel I have no doubt he can make this brand grow and be even more iconic.”
Blake Charlton, MD, then a medical student and now an interventional cardiology fellow at UC-San Francisco, put together a website during an elective project based on input from Verghese and research on the specific skills. They made basic videos of themselves performing the 25, which were posted on the site.
A Further In-Person Enhancement
As the popularity of the Stanford 25 increased, both inside and outside of Stanford, the “bed-med” team sensed a hunger for this applied skill and decided to put on an annual symposium promoting the culture of bedside medicine, with John Kugler taking the lead. The course, now in its fifth year, promised attendees that they would learn to perform and interpret a competent physical exam and, most importantly, to teach advanced physical exam skills at a patient’s bedside.
The popular symposium aims to train clinician-educators who train others at their institutions. “The bedside is where the patients are,” says Verghese, “and we want to show people the joy and renewal that comes from teaching at the bedside and watching students’ eyes open in wonder when we show them how to read the body.”

What Errol has done is truly miraculous, wedding his love of teaching at the bedside with his love of technology
Focusing on the Website
In 2011, then-third-year resident Errol Ozdalga, MD, offered to take over the website, correcting some errors, revamping the website, and expanding the topics and content. He also created a blog and used social media and other venues to promote the content online to drive more traffic to the site. “I thought if it looked good and made sense,” he says, “people would learn from it.”
He made sure it was widely accessible, and he created many new videos, first working with professional videographers and later doing it himself, from storyboarding to filming and editing, often with other faculty. He then migrated the videos to a YouTube channel. He also committed to having a Stanford 25 session during morning report every other week—without fail—which, says Verghese, “is a major undertaking by itself. And he hasn’t deviated.”
Ozdalga, currently clinical associate professor of hospital medicine and director of the Stanford Medicine 25, discusses another aspect of the Stanford 25: “We involve other faculty from neurology, dermatology, ob/gyn, and many faculty from our medicine department. We also have faculty from outside Stanford, including outside the U.S., whom I have filmed to capture how they teach specific exams. I’m in debt to them all for volunteering time to help grow the content on the website and YouTube channel.”
During a Stanford 25 session, a real patient—as opposed to an actor playing the role of a patient—is often brought in, and the instructors focus on a single element of the physical exam to teach the residents. Ozdalga recalls being “super nervous about teaching my fellow residents a particular skill during a Stanford 25 session. Of course, that’s how you learn: You get thrown in the deep water.”
Today the Stanford 25 website has 5,000 visitors daily and is second only to Stanford’s news office in hits for a Stanford website. In the first six months of 2019, the Stanford 25 website had over 1 million page views: 1.068 million to be precise.
Verghese says, “What Errol has done is truly miraculous, wedding his love of teaching at the bedside with his love of technology. The Stanford 25 is already a well-known go-to resource the world over, but with more resources and personnel I have no doubt he can make this brand grow and be even more iconic.”










