
by dom-wp-admin | Feb 27, 2024 | 2023, Rebuilding Community Connections 2023
2023 Annual Report Welcome Department by the Numbers All 2023 Stories Credits Steven Lin, MD Unleashing the Power of AI in Primary Care Steven Lin, MD Unleashing the Power of AI in Primary Care Steven Lin, MD, family physician and section chief of general primary care...

by dom-wp-admin | Feb 27, 2024 | 2023, Clinical Care 2023
2023 Annual Report Welcome Department by the Numbers All 2023 Stories Credits The Clinical Informatics Group uses AI to improve how doctors and nurses identify and assess hospitalized patients at risk of deterioration. Clinical Informatics Harnesses Information...
by dom-wp-admin | Feb 27, 2024 | 2023, Education 2023
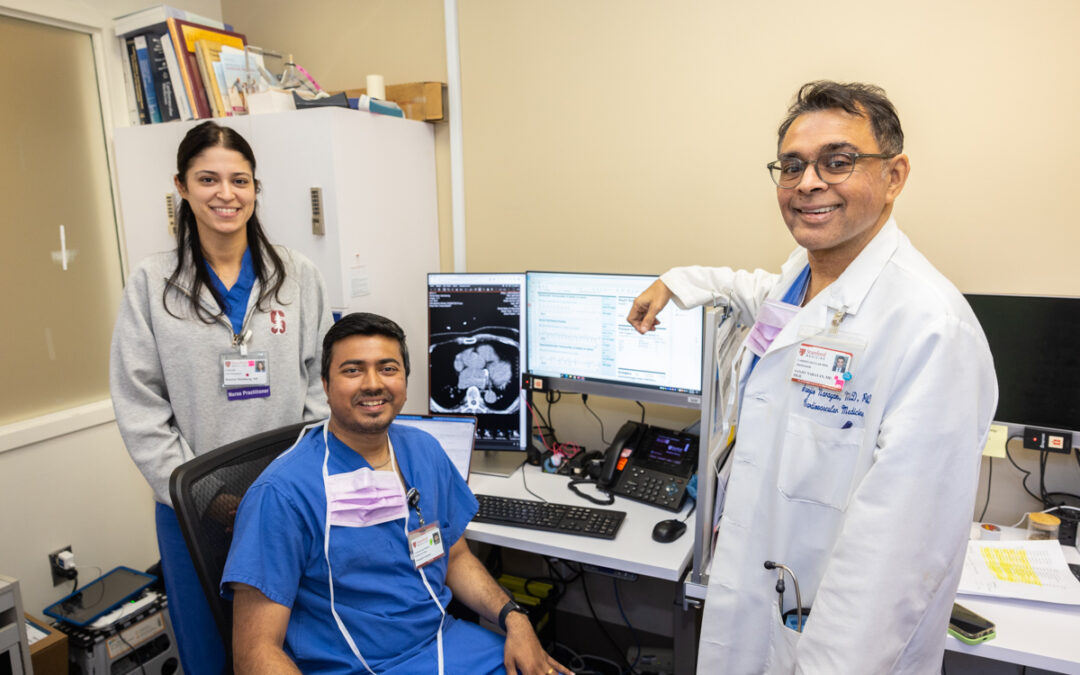
2023 Annual Report Welcome Department by the Numbers All 2023 Stories Credits From left: Desiree Steinberg, NP; Prasanth Ganesan, PhD; and Sanjiv M. Narayan, MD, PhD CHIP: Where Artificial Intelligence and Cardiology Come Together From left: Desiree Steinberg, NP;...




