Paid Summer Internship Program Furthers Stanford Commitment to Diversity, Equity, Inclusion

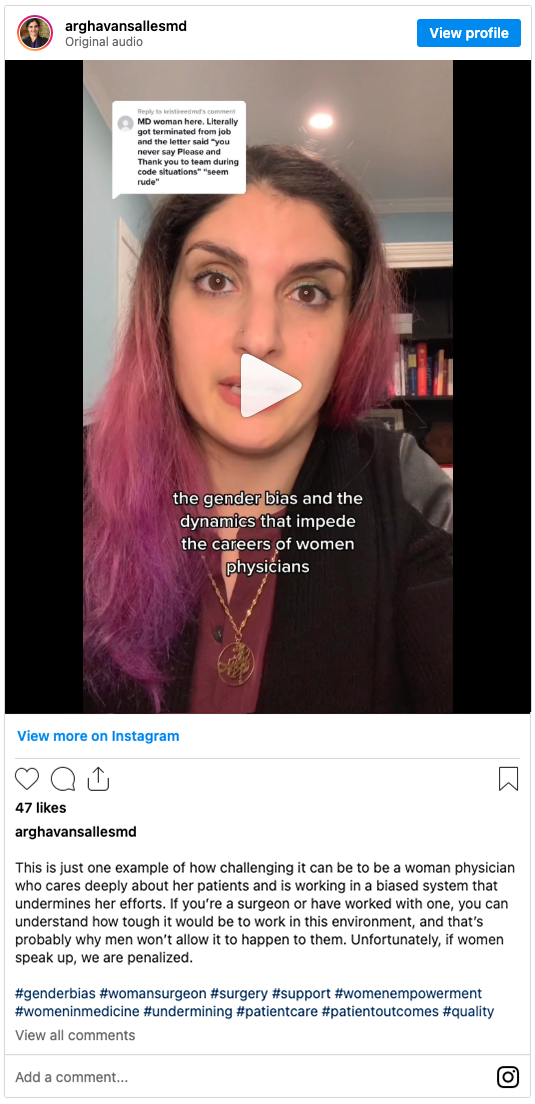
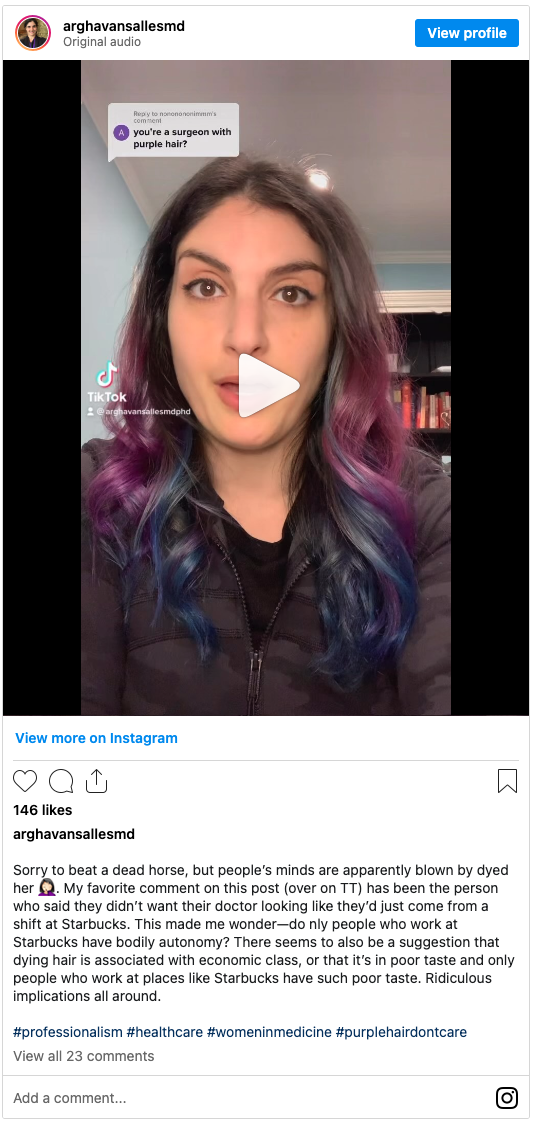
Front row, from left: Josue Parra, UC Berkeley; Briana Giglio, San Jose State University; Sarah Morales, UC Berkeley; Daphney Saviotti-Orozco, UC Berkeley. Back row, from left: Cecile Bonini and Karina Delgado-Carrasco
Paid Summer Internship Program Furthers Stanford Commitment to Diversity, Equity, Inclusion

Front row, from left: Josue Parra, UC Berkeley; Briana Giglio, San Jose State University; Sarah Morales, UC Berkeley; Daphney Saviotti-Orozco, UC Berkeley. Back row, from left: Cecile Bonini and Karina Delgado-Carrasco
Paid Summer Internship Program Furthers Stanford Commitment to Diversity, Equity, Inclusion
During the summer of 2023, the Department of Medicine launched a Paid Internship Program for college students. Through this initiative, eight undergraduates from local universities were placed in staff positions across four divisions in the department.
In the interview that follows, Cecile Bonini, associate director of human resources, and Karina Delgado-Carrasco, director of education programs, answer questions about why the program was established and what it hopes to achieve in the future.
What is the Paid Internship Program?
Bonini: The Paid Internship Program creates summer staff positions for a diverse group of students with a strong appreciation for diversity, equity, inclusion, and belonging (DEIB), who are interested in careers in health care, academic medicine, and administrative roles in higher learning.
How did you go about setting it up?
Bonini: Karina and I reached out to student advisers at local schools and universities to seek applicants with relevant majors. We also contacted campus student support centers and “first-gen” offices, to reach students who were first in their families to attend college.
We promoted the availability of the internships to all 15 divisions in our department. We then developed job descriptions with managers who were excited about supervising a student in a staff role within their work groups.
For this past summer, we had six managers sign on to train and supervise a student. We hired eight people from San Jose State University, UC Berkeley, and the University of San Francisco. Hopefully, these students will view us as a potential employer when they graduate.
What led to the creation of the Paid Internship Program?
Bonini: Two events occurred in 2021. First, the results of a university-wide equity, diversity, and inclusion survey were published. The data showed that though there are spaces at Stanford that can be welcoming and inclusive for many, we have a long way to go as a university to achieve broad-based inclusivity and belonging for all members of the Stanford community.
And second, I noticed that many of the undergraduate students attending our virtual job fairs were asking about paid summer positions. Though we did have summer traineeships available, they were often unpaid or had already been filled by the specific principal investigator seeking those roles.
And how did these two issues motivate you to create this new program?
Bonini: Karina and I felt we could leverage these two scenarios by proactively reaching out to local schools and universities to seek undergraduates who were mission driven; had a strong lens for DEIB; and were interested in health care, academic medicine, or university administration. We would create new summer paid positions with the help of managers who were willing to supervise such individuals on their staff teams.
We approached department leaders who thought this was a wonderful idea. Our director of finance and administration, Cathy Garzio, authorized funding for eight paid summer internships for 2023.
Cecile Bonini (left) and Karina Delgado-Carrasco
Delgado-Carrasco: We also view this program as an opportunity to create a pipeline of candidates who might match a full-time staff role at Stanford in the future. Many students we spoke to were not aware of the numerous employment opportunities we offer; mostly they viewed “health care” as going to medical school or another type of professional training program. Some even thought you had to attend Stanford to work there!
Our goal is to welcome people who otherwise may not have considered working at Stanford and to demonstrate that we have numerous job opportunities for people with a variety of backgrounds and life experiences.
From left: Josue Parra, Briana Giglio, Sarah Morales, Daphney Saviotti-Orozco
During the summer of 2023, the Department of Medicine launched a Paid Internship Program for college students. Through this initiative, eight undergraduates from local universities were placed in staff positions across four divisions in the department.
In the interview that follows, Cecile Bonini, associate director of human resources, and Karina Delgado-Carrasco, director of education programs, answer questions about why the program was established and what it hopes to achieve in the future.
What is the Paid Internship Program?
Bonini: The Paid Internship Program creates summer staff positions for a diverse group of students with a strong appreciation for diversity, equity, inclusion, and belonging (DEIB), who are interested in careers in health care, academic medicine, and administrative roles in higher learning.
How did you go about setting it up?
Bonini: Karina and I reached out to student advisers at local schools and universities to seek applicants with relevant majors. We also contacted campus student support centers and “first-gen” offices, to reach students who were first in their families to attend college.
We promoted the availability of the internships to all 15 divisions in our department. We then developed job descriptions with managers who were excited about supervising a student in a staff role within their work groups.
For this past summer, we had six managers sign on to train and supervise a student. We hired eight people from San Jose State University, UC Berkeley, and the University of San Francisco. Hopefully, these students will view us as a potential employer when they graduate.

Cecile Bonini (left) and Karina Delgado-Carrasco
What led to the creation of the Paid Internship Program?
Bonini: Two events occurred in 2021. First, the results of a university-wide equity, diversity, and inclusion survey were published. The data showed that though there are spaces at Stanford that can be welcoming and inclusive for many, we have a long way to go as a university to achieve broad-based inclusivity and belonging for all members of the Stanford community.
And second, I noticed that many of the undergraduate students attending our virtual job fairs were asking about paid summer positions. Though we did have summer traineeships available, they were often unpaid or had already been filled by the specific principal investigator seeking those roles.
And how did these two issues motivate you to create this new program?
Bonini: Karina and I felt we could leverage these two scenarios by proactively reaching out to local schools and universities to seek undergraduates who were mission driven; had a strong lens for DEIB; and were interested in health care, academic medicine, or university administration. We would create new summer paid positions with the help of managers who were willing to supervise such individuals on their staff teams.
We approached department leaders who thought this was a wonderful idea. Our director of finance and administration, Cathy Garzio, authorized funding for eight paid summer internships for 2023.
Delgado-Carrasco: We also view this program as an opportunity to create a pipeline of candidates who might match a full-time staff role at Stanford in the future. Many students we spoke to were not aware of the numerous employment opportunities we offer; mostly they viewed “health care” as going to medical school or another type of professional training program. Some even thought you had to attend Stanford to work there!
Our goal is to welcome people who otherwise may not have considered working at Stanford and to demonstrate that we have numerous job opportunities for people with a variety of backgrounds and life experiences.

From left: Josue Parra, Briana Giglio, Sarah Morales, Daphney Saviotti-Orozco

The Paid Internship Program creates summer staff positions for a diverse group of students with a strong appreciation for diversity, equity, inclusion, and belonging, who are interested in careers in health care, academic medicine, and administrative roles in higher learning.
— Cecile Bonini, associate director of human resources
What did this year’s participants do?
Bonini: The eight students worked in various roles in clinical research and administrative support. But it wasn’t all work: We had four professional development seminars that highlighted the importance of personal branding, self-awareness, and networking. Stanford comes with a reputation that some people can find intimidating, so we tried to help the students navigate the organization, ideally so they could envision themselves in full-time roles here in the future. And we had a lovely closing session at the end of the summer, where we bid the students farewell and invited them to keep in touch with one another and with the various connections they made during their time here.
Why do you feel this program is important?
Delgado-Carrasco: Thinking back on my own career journey, I believe having an opportunity like this would have helped me see that there was so much more to do “out there” than I knew about when I was in school. I was a public health major as an undergraduate, but I really didn’t know what that meant in terms of the multiple options I would have for career choices. I felt a little lost back then! I hope this program helps participants understand the numerous roles people who are interested in health care can play.

The Paid Internship Program creates summer staff positions for a diverse group of students with a strong appreciation for diversity, equity, inclusion, and belonging, who are interested in careers in health care, academic medicine, and administrative roles in higher learning.
— Cecile Bonini, associate director of human resources
What did this year’s participants do?
Bonini: The eight students worked in various roles in clinical research and administrative support. But it wasn’t all work: We had four professional development seminars that highlighted the importance of personal branding, self-awareness, and networking. Stanford comes with a reputation that some people can find intimidating, so we tried to help the students navigate the organization, ideally so they could envision themselves in full-time roles here in the future. And we had a lovely closing session at the end of the summer, where we bid the students farewell and invited them to keep in touch with one another and with the various connections they made during their time here.
Why do you feel this program is important?
Delgado-Carrasco: Thinking back on my own career journey, I believe having an opportunity like this would have helped me see that there was so much more to do “out there” than I knew about when I was in school. I was a public health major as an undergraduate, but I really didn’t know what that meant in terms of the multiple options I would have for career choices. I felt a little lost back then! I hope this program helps participants understand the numerous roles people who are interested in health care can play.