Where Health Care Is a Luxury
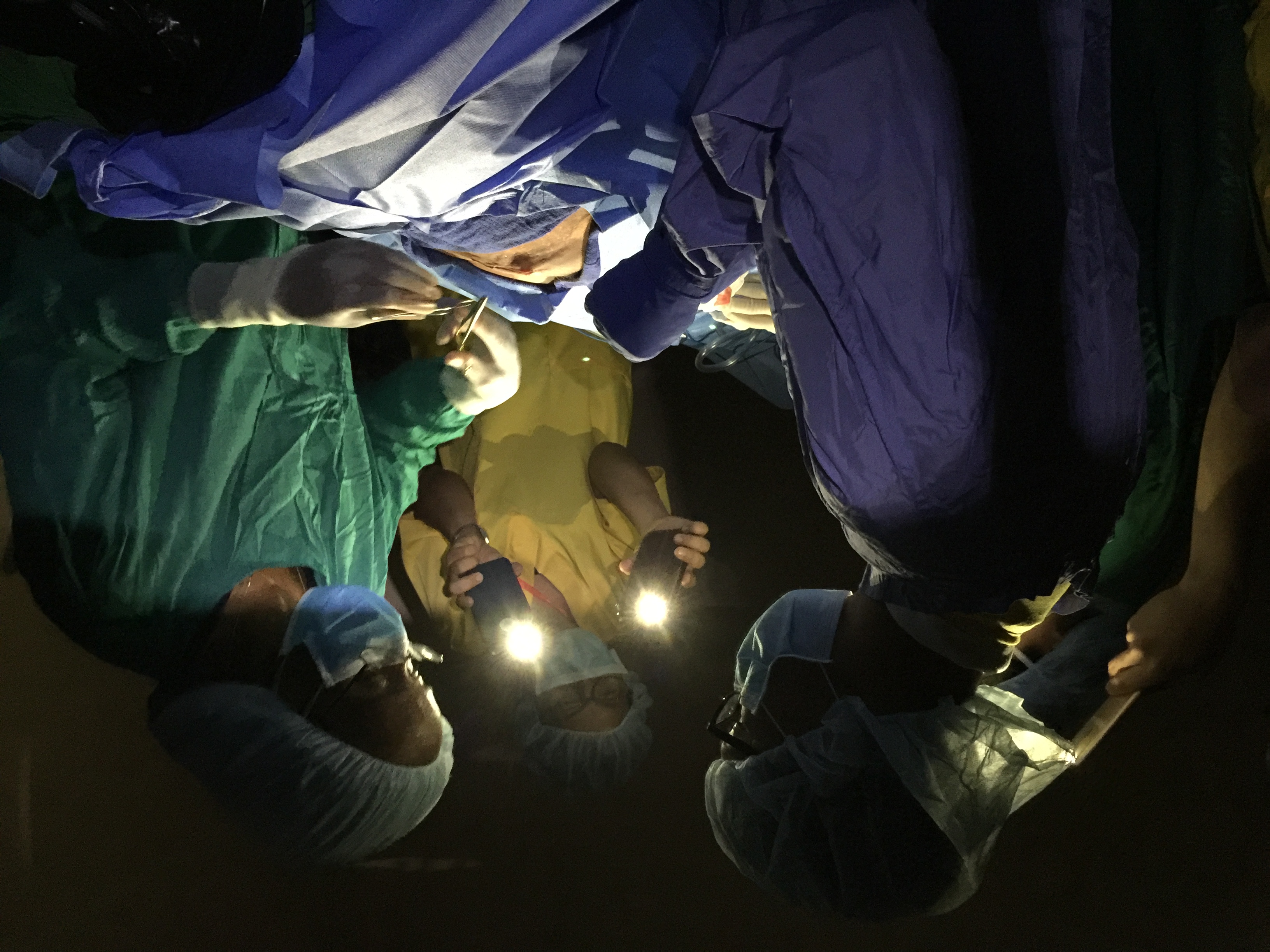
Power failures are common in rural Cambodia. One that occurred during surgery required improvisation, with several mobile phones providing light.
Where Health Care Is a Luxury

Power failures are common in rural Cambodia. One that occurred during surgery required improvisation, with several mobile phones providing light.
Where Health Care Is a Luxury
Take a 24-hour flight to Phnom Penh, Cambodia. Board a bus and ride for 10 hours to the rural province of Banteay Meanchey. Help set up medical, surgical, dental, and ophthalmological outpatient clinics. See more than 100 patients a day. A week later, take it all apart and fly home. Repeat in a year.
Though he visits a different village every year, that’s the annual routine that Robert Negrin, MD, has followed for the past 10 years, except for a three-year hiatus due to the COVID-19 pandemic. “It’s wonderful to reconnect with my friends and colleagues each year,” he notes. “We have an incredible camaraderie, and we all missed each other during the pandemic gap.”
Negrin, a professor of blood and marrow transplantation medicine, volunteers in the yearly medical missions sponsored by the Cambodian Health Professionals Association of America (CHPAA). About 100 people participate, of which 30 are physicians. “We work with patients, medical students, and others in an environment where health care is a luxury if and when it is even available,” he says.
Trained as a hematologist, Negrin serves as a general medical physician in the clinic in Cambodia, referring patients to the surgery, dental, or ophthalmology team members as needed — in a similar fashion to the subspecialty referrals that primary care physicians make at Stanford.
Medical Students Eager for Knowledge
In addition to seeing hundreds of patients on each trip, Negrin and his colleagues enjoy working with the Cambodian medical students who serve as interpreters. “They are all dying for interactions with us,” says Negrin. “They are like sponges: bright, committed, dedicated, and eager to learn about American medicine.”
In fact, some of the medical students Negrin has worked with in the past are now physicians themselves. “They are the ones who will change health care in Cambodia and go on to help take care of their own people,” he says, adding that “an improved healthcare system in Cambodia would make the need for these medical missions unnecessary.”
But right now, the need is enormous, especially in rural areas where thousands of people line up for 10 hours or more every day of the weeklong medical mission to be seen by a physician. “What is remarkable,” Negrin observes, “is that no one complains about the wait, or how hot it is, or that they didn’t get to be seen.”
Two Patients Remembered
Over the course of his 10 years as a volunteer with CHPAA, Negrin has seen thousands of patients. Although many are memorable, two stand out in his mind.
A 22-year-old woman came to the clinic looking “as white as a ghost,” he recalls. He ordered some blood tests but couldn’t make an accurate diagnosis. He raised money through GoFundMe to send her to Bangkok, Thailand, where hospital staff determined that she had leukemia. Her treatment there resulted in a four-year remission. She and her husband came to the mission site each year, even though it was often a great distance from their home. They adopted a child and became close friends with Negrin. Then, she unfortunately suffered a relapse, and though Negrin tried to get her to China for care, he was not able to do so. Sadly, she passed away.
“This was difficult for me because I had to accept the limitations in the Cambodian healthcare system and that I couldn’t do everything I knew I could have done for her,” he says. “I still think about her and am saddened by the harshness of fate that is so impacted by where you happen to have been born.”
A second memory is of a woman in her late 20s who came to see him but was embarrassed to have him examine her. With the help of a Cambodian female medical student, she allowed him to proceed. He found a lump in her breast. The woman told him that it made her feel like she wasn’t a true woman. Negrin helped collect money from CHPAA volunteers to send her to see a physician who had participated in the CHPAA program as a medical student and was now in practice in Phnom Penh. There, through their generosity, she was able to undergo surgery to remove the tumor. Later, she sent Negrin a photo of her wedding and told him that she felt like a full woman again.
Hundreds of patients from Cambodian rural villages wait for as long as 10 hours every day of the annual weeklong medical mission sponsored by the Cambodian Health Professionals Association of America. Volunteer Robert S. Negrin, MD, professor of blood and marrow transplantation medicine, comments that “no one complains about the wait, or how hot it is, or that they didn’t get to be seen.”

Take a 24-hour flight to Phnom Penh, Cambodia. Board a bus and ride for 10 hours to the rural province of Banteay Meanchey. Help set up medical, surgical, dental, and ophthalmological outpatient clinics. See more than 100 patients a day. A week later, take it all apart and fly home. Repeat in a year.
Though he visits a different village every year, that’s the annual routine that Robert Negrin, MD, has followed for the past 10 years, except for a three-year hiatus due to the COVID-19 pandemic. “It’s wonderful to reconnect with my friends and colleagues each year,” he notes. “We have an incredible camaraderie, and we all missed each other during the pandemic gap.”
Negrin, a professor of blood and marrow transplantation medicine, volunteers in the yearly medical missions sponsored by the Cambodian Health Professionals Association of America (CHPAA). About 100 people participate, of which 30 are physicians. “We work with patients, medical students, and others in an environment where health care is a luxury if and when it is even available,” he says.
Trained as a hematologist, Negrin serves as a general medical physician in the clinic in Cambodia, referring patients to the surgery, dental, or ophthalmology team members as needed — in a similar fashion to the subspecialty referrals that primary care physicians make at Stanford.
Medical Students Eager for Knowledge
In addition to seeing hundreds of patients on each trip, Negrin and his colleagues enjoy working with the Cambodian medical students who serve as interpreters. “They are all dying for interactions with us,” says Negrin. “They are like sponges: bright, committed, dedicated, and eager to learn about American medicine.”
In fact, some of the medical students Negrin has worked with in the past are now physicians themselves. “They are the ones who will change health care in Cambodia and go on to help take care of their own people,” he says, adding that “an improved healthcare system in Cambodia would make the need for these medical missions unnecessary.”
But right now, the need is enormous, especially in rural areas where thousands of people line up for 10 hours or more every day of the weeklong medical mission to be seen by a physician. “What is remarkable,” Negrin observes, “is that no one complains about the wait, or how hot it is, or that they didn’t get to be seen.”

Hundreds of patients from Cambodian rural villages wait for as long as 10 hours every day of the annual weeklong medical mission sponsored by the Cambodian Health Professionals Association of America. Volunteer Robert S. Negrin, MD, professor of blood and marrow transplantation medicine, comments that “no one complains about the wait, or how hot it is, or that they didn’t get to be seen.”
Two Patients Remembered
Over the course of his 10 years as a volunteer with CHPAA, Negrin has seen thousands of patients. Although many are memorable, two stand out in his mind.
A 22-year-old woman came to the clinic looking “as white as a ghost,” he recalls. He ordered some blood tests but couldn’t make an accurate diagnosis. He raised money through GoFundMe to send her to Bangkok, Thailand, where hospital staff determined that she had leukemia. Her treatment there resulted in a four-year remission. She and her husband came to the mission site each year, even though it was often a great distance from their home. They adopted a child and became close friends with Negrin. Then, she unfortunately suffered a relapse, and though Negrin tried to get her to China for care, he was not able to do so. Sadly, she passed away.
“This was difficult for me because I had to accept the limitations in the Cambodian healthcare system and that I couldn’t do everything I knew I could have done for her,” he says. “I still think about her and am saddened by the harshness of fate that is so impacted by where you happen to have been born.”
A second memory is of a woman in her late 20s who came to see him but was embarrassed to have him examine her. With the help of a Cambodian female medical student, she allowed him to proceed. He found a lump in her breast. The woman told him that it made her feel like she wasn’t a true woman. Negrin helped collect money from CHPAA volunteers to send her to see a physician who had participated in the CHPAA program as a medical student and was now in practice in Phnom Penh. There, through their generosity, she was able to undergo surgery to remove the tumor. Later, she sent Negrin a photo of her wedding and told him that she felt like a full woman again.

It’s the human contact with the patients and especially the students, many of whom have become lifelong friends. And the knowledge that I’ve made a small impact on the lives of a few people. I know we are just Band-Aids in the big picture, but lately I’ve stopped asking myself why I do this.
We Are So Privileged in the U.S.
Negrin says that the hardest part of each of the trips is coming home. “We are so privileged here in the United States,” he says. “I start to question why are we ordering a CT scan for every little thing? What is the likelihood we will find anything significant? At times, the care we provide is so excessive. It’s made me reevaluate how I function as a clinician in a healthcare system that is rich in resources and the finest in the world.”
Why does Negrin keep going back? “It’s the human contact with the patients and especially the students, many of whom have become lifelong friends,” he says. “And the knowledge that I’ve made a small impact on the lives of a few people. I know we are just Band-Aids in the big picture, but lately I’ve stopped asking myself why I do this.”

Volunteers from the Cambodian Health Professionals Association of America medical mission, with Robert S. Negrin, MD, professor of blood and marrow transplantation medicine (seated on red stool) and Cambodian medical students who serve as interpreters (wearing yellow shirts).

It’s the human contact with the patients and especially the students, many of whom have become lifelong friends. And the knowledge that I’ve made a small impact on the lives of a few people. I know we are just Band-Aids in the big picture, but lately I’ve stopped asking myself why I do this.
We Are So Privileged in the U.S.
Negrin says that the hardest part of each of the trips is coming home. “We are so privileged here in the United States,” he says. “I start to question why are we ordering a CT scan for every little thing? What is the likelihood we will find anything significant? At times, the care we provide is so excessive. It’s made me reevaluate how I function as a clinician in a healthcare system that is rich in resources and the finest in the world.”
Why does Negrin keep going back? “It’s the human contact with the patients and especially the students, many of whom have become lifelong friends,” he says. “And the knowledge that I’ve made a small impact on the lives of a few people. I know we are just Band-Aids in the big picture, but lately I’ve stopped asking myself why I do this.”

Volunteers from the Cambodian Health Professionals Association of America medical mission, with Robert S. Negrin, MD, professor of blood and marrow transplantation medicine (seated on red stool) and Cambodian medical students who serve as interpreters (wearing yellow shirts).






















