Two Residents, United in Equality, Are Fighting Health Disparities

Two Residents, United in Equality, Are Fighting Health Disparities
As medical residents, Christine Santiago, MD, and Natasha Steele, MD, helped shape the narrative along the halls of Stanford and beyond when it came to equity, diversity, and hands-on experience in health care. Now as recently appointed assistant professors in the Department of Medicine, both are using their voices to bring positive change to patients of all races, backgrounds, abilities, and income levels. The idea that we become who we need rings true for both professors, and their shared experiences of having ill family members, navigating the healthcare system, and serving side by side have created a new sisterhood that will impact them and others for years to come.

Two Residents, United in Equality, Are Fighting Health Disparities

Christine Santiago, MD
Santiago has been bridging the gap in health care since elementary school in New York City. There, she witnessed the devastating impact on her family and community when medical providers didn’t view health care through the same cultural lens as the community they served.

Natasha Z.R. Steele, MD
For some, a career in medicine stems from life experience and wanting to help others, but what happens when you become your own case study?
As medical residents, Christine Santiago, MD, and Natasha Steele, MD, helped shape the narrative along the halls of Stanford and beyond when it came to equity, diversity, and hands-on experience in health care. Now as recently appointed assistant professors in the Department of Medicine, both are using their voices to bring positive change to patients of all races, backgrounds, abilities, and income levels. The idea that we become who we need rings true for both professors, and their shared experiences of having ill family members, navigating the healthcare system, and serving side by side have created a new sisterhood that will impact them and others for years to come.

Christine Santiago, MD
Santiago has been bridging the gap in health care since elementary school in New York City. There, she witnessed the devastating impact on her family and community when medical providers didn’t view health care through the same cultural lens as the community they served.

Natasha Z.R. Steele, MD
For some, a career in medicine stems from life experience and wanting to help others, but what happens when you become your own case study?
Christine Santiago: Challenge Accepted
Santiago has been bridging the gap in health care since elementary school in New York City. There, she witnessed the devastating impact on her family and community when medical providers didn’t view health care through the same cultural lens as the community they served. She regularly translated medical jargon for family members who struggled to understand their medical conditions, medications, and follow-up care.
During those early childhood years, she decided to pursue a medical career, but her college counselor told her that medical school wasn’t an option and to find another profession.
Undaunted, Santiago went on to graduate from Harvard Medical School cum laude and UC Berkeley with a Master’s in Public Health.
Meeting Wendy Caceres, MD, of the Stanford Clinical Opportunity for Residency Experience (SCORE) program, made a significant impact on Santiago. Caceres, a clinical associate professor of primary care and population health, knew SCORE would offer Santiago the depth of knowledge and experience needed to treat patients of varying needs and backgrounds in real time.

Christine Santiago, MD

Christine Santiago, MD
Christine Santiago: Challenge Accepted
Santiago has been bridging the gap in health care since elementary school in New York City. There, she witnessed the devastating impact on her family and community when medical providers didn’t view health care through the same cultural lens as the community they served. She regularly translated medical jargon for family members who struggled to understand their medical conditions, medications, and follow-up care.
During those early childhood years, she decided to pursue a medical career, but her college counselor told her that medical school wasn’t an option and to find another profession.
Undaunted, Santiago went on to graduate from Harvard Medical School cum laude and UC Berkeley with a Master’s in Public Health.
Meeting Wendy Caceres, MD, of the Stanford Clinical Opportunity for Residency Experience (SCORE) program, made a significant impact on Santiago. Caceres, a clinical associate professor of primary care and population health, knew SCORE would offer Santiago the depth of knowledge and experience needed to treat patients of varying needs and backgrounds in real time.

She regularly translated medical jargon for family members who struggled to understand their medical conditions, medications, and follow-up care.
While a resident at Stanford, Santiago wanted answers and solutions when her father broke a bone and had trouble getting opioids to dull the pain — because the doctors thought he would become addicted. It is not uncommon for this to happen to people of color with little to no recourse, Santiago says.
She responded to her concerns by co-founding Internal Medicine Health Equity, Advocacy and Research (IM HEARs) in 2020 with fellow resident Gabriela Spencer Bonilla, MD.
“The program aims to develop internists who are committed to the care of disadvantaged and vulnerable populations within the United States. It started with three residents and has grown to 18 residents dedicated to creating better health care outcomes while building stronger community ties,” says Santiago.
Now an assistant professor of hospital medicine, Santiago has the same goal as she had in her youth: to create better health outcomes for all — regardless of race, culture, education, sexual orientation, religion, or finances.
Natasha Steele: A Challenging Diagnosis
For some, a career in medicine stems from life experience and wanting to help others, but what happens when you become your own case study?
Eleven days after arriving at Stanford as an intern, Steele discovered that she had Hodgkin lymphoma. She would now fight two battles: cancer and a healthcare system that was not always inclusive.
Steele grew up in a large immigrant family with a Moroccan mother and an American father. Her familial background reflected two worlds — family with medical access and family without. It was startling: There were biases all around, and it shaped how Steele would navigate the world. She eventually earned a Master’s in Public Health from George Washington University and a medical degree from the University of Washington to tackle systemic issues in healthcare from different angles.
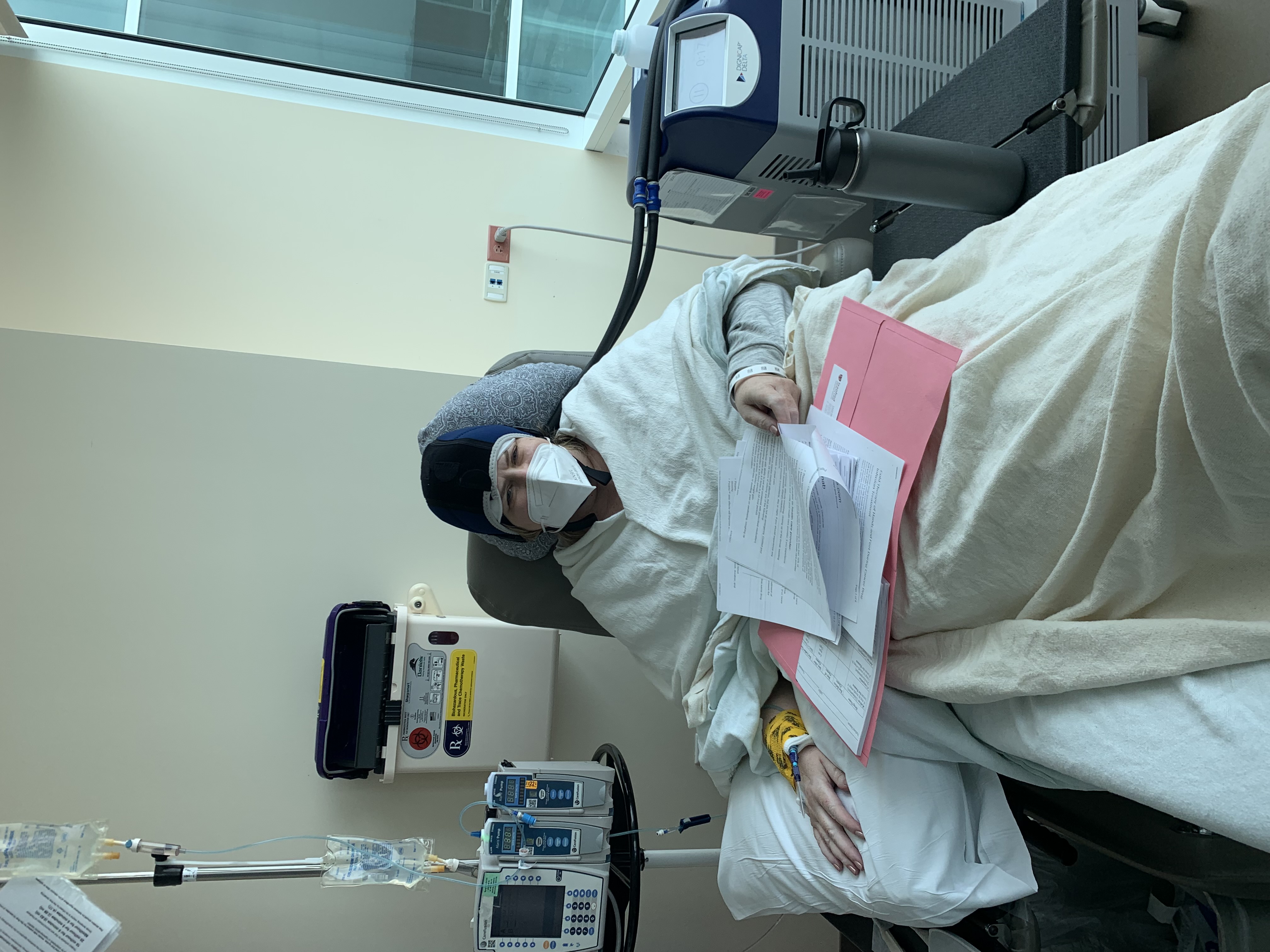
Steele believes her experience with cancer gave more than it took.

Natasha Steele, MD, believes her experience with cancer gave more than it took

Natasha Steele, MD, believes her experience with cancer gave more than it took
Natasha Steele: A Challenging Diagnosis
For some, a career in medicine stems from life experience and wanting to help others, but what happens when you become your own case study?
Eleven days after arriving at Stanford as an intern, Steele discovered that she had Hodgkin lymphoma. She would now fight two battles: cancer and a healthcare system that was not always inclusive.
Steele grew up in a large immigrant family with a Moroccan mother and an American father. Her familial background reflected two worlds — family with medical access and family without. It was startling: There were biases all around, and it shaped how Steele would navigate the world. She eventually earned a Master’s in Public Health from George Washington University and a medical degree from the University of Washington to tackle systemic issues in healthcare from different angles.
Steele believes her experience with cancer gave more than it took.

When I returned to residency after my diagnosis, I found that I had a firsthand perspective on the challenges my patients faced, the sanctity of the physician-patient bond, and the need to train physicians to be patient advocates.
“When I returned to residency after my diagnosis, I found that I had a firsthand perspective on the challenges my patients faced, the sanctity of the physician-patient bond, and the need to train physicians to be patient advocates. I was looking for a community of doctors at Stanford who might share this perspective and found Stanford Medicine Alliance for Disability Inclusion and Equity (SMADIE). This is an incredible group of med students, residents, fellows, and medical faculty who have all faced disability or illness in some way and are changing the game when it comes to advocacy and awareness for these issues,” says Steele.
Around the same time, she met her mentor, Lidia Schapira, MD, professor of oncology and director of the Stanford Cancer Survivorship Program. Schapira brought Steele into the fold of the cancer survivorship community, and together they have teamed up on research and creative endeavors like “Health After Cancer,” a Stanford podcast that features storytelling by cancer survivors and medical experts to create community and shared experience.
In addition, Steele was and continues to be active in IM HEARs, the Stanford Medicine Diversity Committee, and the Women in Internal Medicine Residency Group.
In April 2023, Steele spoke to the American Association of Medical Colleges about “the critical value of training doctors who have diverse illness experiences — how these medical providers often make the fiercest, most empathetic advocates for their patients,” said Steele.
For that presentation, and now as assistant professor of hospital medicine, she clearly uses her full life story to create better health outcomes for anyone she meets.