Embracing a Growing Community of Advanced Practice Providers
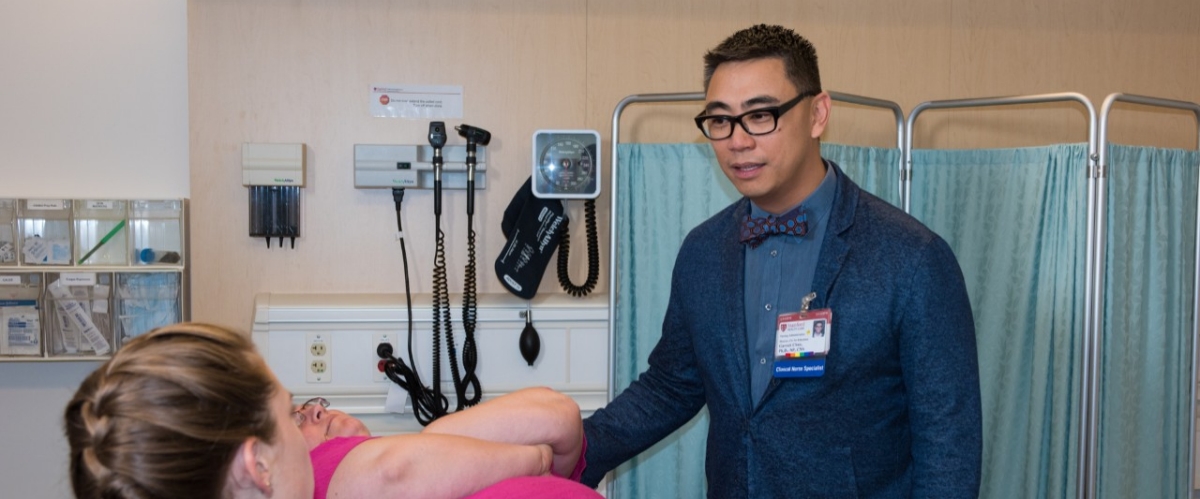
Garrett Chan, PhD, RN, teaching in a simulation lab.
Embracing a Growing Community of Advanced Practice Providers

Garrett Chan, PhD, RN, teaching in a simulation lab.
Embracing a Growing Community of Advanced Practice Providers
Garrett Chan, PhD, a clinical associate professor of primary care and population health and emergency medicine, spent his 20s pursuing a career as an art curator, taking classes like art history and humanities, with the eventual goal of working at a museum.
But then he met with a counselor, who prompted him to scrap the curatorial track and explore a career in nursing. Chan was surprisingly receptive. “I said sure!” he explains, “so she handed me a paper with a list of courses like chemistry, anatomy, and biology.” Clutching his new curriculum, he set off to embark on an entirely new path.
Chan spent the next several years acquiring degrees (an RN and BSN from San José State and a MS and PhD from UC-San Francisco), and clinical experience (in the emergency department and palliative care services of the San Jose Medical Center and at Stanford) at breakneck speed.
He joined Stanford Health Care as a nurse-scientist in 2006, and the Department of Medicine as a faculty member in 2014. Chan is not exclusively a nurse. His interests—and identities—vary widely. “My daily work as a faculty member includes administration in Stanford Health Care, direct care of patients, and work as a research scientist and an educator.”
On any given day, he can be found in the emergency department, helping faculty evaluate the efficacy of a new critical care program; in the lab, acting as principal investigator on a multi-site clinical trial of an FDA-approved device designed to test subepidermal moisture and writing up the results; in the office, creating curriculum for an RN postdoctoral fellowship in palliative care; or in the classroom, leading the advanced practice provider fellowship program and training interdisciplinary staff as the director of the Center for Professional Development.
Garrett Chan, PhD, a clinical associate professor of primary care and population health and emergency medicine, spent his 20s pursuing a career as an art curator, taking classes like art history and humanities, with the eventual goal of working at a museum.
But then he met with a counselor, who prompted him to scrap the curatorial track and explore a career in nursing. Chan was surprisingly receptive. “I said sure!” he explains, “so she handed me a paper with a list of courses like chemistry, anatomy, and biology.” Clutching his new curriculum, he set off to embark on an entirely new path.
Chan spent the next several years acquiring degrees (an RN and BSN from San José State and a MS and PhD from UC-San Francisco), and clinical experience (in the emergency department and palliative care services of the San Jose Medical Center and at Stanford) at breakneck speed.

They bring a very HOLISTIC perspective to health care.
He joined Stanford Health Care as a nurse-scientist in 2006, and the Department of Medicine as a faculty member in 2014. Chan is not exclusively a nurse. His interests—and identities—vary widely. “My daily work as a faculty member includes administration in Stanford Health Care, direct care of patients, and work as a research scientist and an educator.” On any given day, he can be found in the emergency department, helping faculty evaluate the efficacy of a new critical care program; in the lab, acting as principal investigator on a multi-site clinical trial of an FDA-approved device designed to test subepidermal moisture and writing up the results; in the office, creating curriculum for an RN postdoctoral fellowship in palliative care; or in the classroom, leading the advanced practice provider fellowship program and training interdisciplinary staff as the director of the Center for Professional Development.
Chan is also part of a growing community of advanced-practice providers—including registered nurses, nurse practitioners, and physician assistants—working alongside medical doctors on campus. There are several nurse scientists employed by the department. And in August Stanford welcomed the inaugural class of 27 students in the master of science in physician assistant studies program. It’s an exciting and beneficial shift, Chan explains. “A significant part of physician education and practice is focused on disease management,” he says. “And while nurses always have disease management in mind, they bring a very holistic perspective to health care. We’re paying attention to how patients and families are coping, patient education, and other psycho-social aspects of care.” Chan predicts that the inclusion of different care perspectives will both complement—and enhance—the practice of medicine and delivery of health care at Stanford.

They bring a very HOLISTIC perspective to health care.
Chan is also part of a growing community of advanced-practice providers—including registered nurses, nurse practitioners, and physician assistants—working alongside medical doctors on campus. There are several nurse scientists employed by the department. And in August Stanford welcomed the inaugural class of 27 students in the master of science in physician assistant studies program. It’s an exciting and beneficial shift, Chan explains. “A significant part of physician education and practice is focused on disease management,” he says. “And while nurses always have disease management in mind, they bring a very holistic perspective to health care. We’re paying attention to how patients and families are coping, patient education, and other psycho-social aspects of care.” Chan predicts that the inclusion of different care perspectives will both complement—and enhance—the practice of medicine and delivery of health care at Stanford.