Endocrine Tumor Program Brings Unparalleled Clinical and Research Expertise Under One Roof


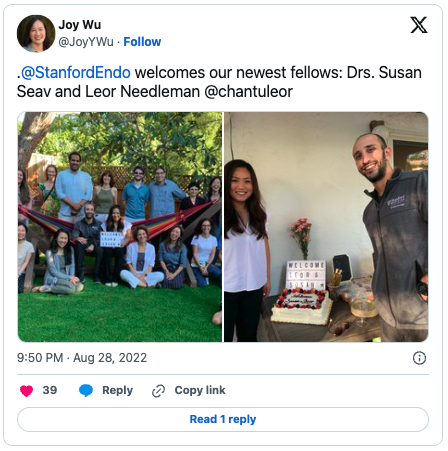
Justin P. Annes, MD, PhD, specializes in rare neuroendocrine tumors called pheo paras.
Endocrine Tumor Program Brings Unparalleled Clinical and Research Expertise Under One Roof
The pheo-para program is a standout example of what can be accomplished when highly skilled and knowledgeable people who are deeply dedicated to an oft-overlooked problem come together with a mission. Co-directed by Justin P. Annes, MD, PhD, associate professor of endocrinology at Stanford, and surgeon Electron Kebebew, MD, the program was recently designated a Pheo Para Research & Clinical Center of Excellence by the Pheo Para Alliance (PPA).
A Lonely and Isolating Diagnosis
“When you’re diagnosed with a rare condition, there’s not only an overwhelming sense of I don’t know what to do but also My physicians don’t know what this is, and they don’t know how to treat it,” says Annes. “It’s really isolating for patients to receive a rare diagnosis, and that’s assuming that the diagnosis can even be made, because oftentimes, particularly for pheo paras, the delay in diagnosis is estimated to be around five years.” This delay is due to the rarity of the condition, a lack of knowledge among nonspecialists, and the fact that symptoms mimic much more common diseases, such as hypertension or anxiety. Such delays mean patients go years without appropriate treatment while the tumors grow, some of which are cancerous.
“The most important thing is to have a center of expertise, where patients have a home where they feel that someone understands their disease, can provide information about their diagnosis, and give them that comfort,” says Annes. “Having leadership in surgery and in medicine also empowers the center, because you have multidepartmental collaboration, which extends to pediatrics as well.”
Putting the Pieces Together with Multidisciplinary Expertise
Pheo paras are complex to treat as well as diagnose. Symptoms and management are highly individualized, depending on where the tumor is located.
“It really requires a collaborative, interdisciplinary team. You need experts across the board, not only in medicine, genetics, and endocrinology, but also in surgery and radiation oncology,” explains Annes. “There are multiple modalities for treatment, like targeted radiopharmaceutical therapy and robot-assisted surgery. It’s really critical that all of these pieces fit together and that your center has all the expertise to really provide patients with the level of knowledge and care that each individual demands. We’ve put that together here.”
Importantly, 35% to 40% of pheo para cases are familial, so truly comprehensive treatment requires the capacity to do genetic testing. The scope of the genetic link has been fully understood for only about a decade, so there is a need to test patients who were diagnosed years ago, along with their families.
“We really want to provide a home, not only for individuals, but for whole families,” says Annes. “An important effort of our center is to not only look forward, but to make sure all of our patients who are cared for at Stanford receive the highest level of care.”
 “The most important thing is to have a center of expertise, where patients have a home where they feel that someone understands their disease, can provide information about their diagnosis, and give them that comfort.” – Justin P. Annes, MD, PhD
“The most important thing is to have a center of expertise, where patients have a home where they feel that someone understands their disease, can provide information about their diagnosis, and give them that comfort.” – Justin P. Annes, MD, PhD
Nose-to-Tail Approach
But that’s not all. The Endocrine Tumor program boasts a cutting-edge research team, offering patients access to experimental treatments through clinical trials. They also conduct in vitro and animal research that drives fundamental discoveries into the molecular underpinnings of these tumors, an area of research that typically bears fruit not just for pheo paras but also for other, more common tumors that have similar genetic and molecular drivers. This kind of nose-to-tail expertise, from basic research to experimental therapeutics, with routine clinical care in between, is rarely seen under one roof for any disease.
“We’re providing state-of-the-art care at the highest level, but we also want to be the ones to make the breakthroughs to provide the next standard of care,” says Annes. “That’s where I’m hoping we can attract more interest, people who are committed to seeing Stanford maintain its level of excellence across not only common disease, but rare diseases as well.”
An example is a recently published research paper by Annes and his team on a study of a newly developed gene panel that will help determine whether specific gene variants influence the risk of developing pheo paras. As of now, many genes associated with the disease remain “of unknown significance.”
Increased Visibility Means More Patients, More Collaboration, New Hope
The Center of Excellence designation from the PPA has increased the visibility of the program among pharmaceutical companies interested in developing novel therapeutics. It has also boosted referrals from both patients and physicians, hopefully increasing the proportion of people with pheo paras who receive a timely diagnosis and appropriate treatment.
Supporting Patients Throughout Their Healthcare Journey
An important goal for Annes and his team is to ensure that patients receive the support they need throughout their healthcare journey. “People undervalue the logistics that patients face when they have a complicated condition like this,” he says. “We have a nurse navigator, who guides patients through the process of their new diagnosis and a very complicated medical system.”
Jill Shugart, 64, of Winters, California, came under the care of Annes after genetic testing revealed that she was at elevated risk for hereditary pheo paras. He identified a growth on her adrenal gland that testing suggested was noncancerous. After several years of monitoring, she elected to have it surgically removed in an abundance of caution, at the recommendation of Annes and Kebebew. Sure enough, it was indeed cancerous, but the surgery appears to have been curative, and she continues to undergo monitoring.
Despite the rarity of her condition, Shugart had to fight with her insurance company and primary care provider through patient advocacy to access the specialized care only available at Stanford. “I am so grateful I was hooked up with Dr. Annes and Dr. Kebebew,” she says. “I felt like I was really being catered to.” After surgery, she asked Annes, “Are we done? Can you keep seeing me?” He said, “Oh, we’re friends for life now.”
“Anywhere in the world I could be, this is where I would want to be – at Stanford,” says Shugart. Had she not been referred to Annes, she speculates, “I wouldn’t have known what I was missing out on. [My previous doctors] may have never caught it. They told me the surgery I had was a very high-risk surgery. I would not have been comfortable doing that at [a nonspecialized center]. When I went into my surgery, I was shocked by how many people were in there. I think I had 27 people on my team.”